UPDATE: Just last week, news broke through that Rinne's issue was worse than previously thought. On November 5th, Sportsnet's Nick Kypreos reported that Rinne's issue was a very dangerous E. Coli infection. Kypreos added that the issue could keep Rinne out until around Christmas (6-8 weeks) instead of the original prognosis of sidelining him for one month.
BACKGROUND
Last summer, it was revealed that Rinne would undergo a hip arthroscopy to correct deterioration in the joint on his left side. Predators GM David Poile stated that the procedure was preventative and that the team's medical staff had been aware of Rinne's hip problems since the end of the 2011-2012 season.
A hip arthroscopy is not an uncommon surgery, especially among NHL players. Tiny holes are made in the surrounding area of the joint, small cameras are inserted and the orthopedic surgeon inserts instruments to clear up or repair the joint. Poile attributed the injury to the workload and play style of modern NHL goaltenders, stating "This, I think, just goes to the position that he's playing, the wear and tear that goaltenders [endure] and what the current style of play is...This is an operation that many, many players in the NHL have had." Rinne was certainly a workhorse the 2012-2013 season, playing in 43 of Nashville's 48 games. Rinne has appeared in 85% of the team's regular-season games as well as 22 playoff games the last two seasons.
Rinne underwent the surgery, performed by Nashville-based orthopedist Dr. Thomas Byrd. Rinne apparently didn't have much discomfort, but after speaking with several doctors and other NHL players that have had the surgery, decided that it was best for his career and quality of life to take care of the deterioration via surgery during the offseason. Rinne's timeline for recovery was the standard four months, and he met that timeline, appearing in Nashville's 2013-2014 season opener.
BREAKING DOWN THE HIP ARTHROSCOPY
As shown in Figure 1 below, the hip is a ball-and-socket joint. The 'ball' is the femoral head (the top of the femur or thighbone) sits in the 'socket' which is formed by the acetabulum, part of the pelvis bone. Articular cartilage covers the surface of the bones in the joint, creating a smooth, frictionless surface which aids the bones glide across each other during movement.
The acetabulum is surrounded by the labrum, a strong fibrocartilage (meaning it is flexible and tough but also has some elasticity). The labrum is analogous to the knee meniscus and the shoulder labrum.The labrum acts as a gasket, sealing in fluid and the joint together as well as helping deepen the socket. The joint is also surround by bands of tissues called ligaments which form a tough capsule and help hold the hip together. The capsule is lined by a thin membrane called the synovium which produces synovial fluid, lubricating the hip joint. The capsule helps contain the joint fluid and maintain cartilage lubrication and nutrition.
Figure 1: The Hip Joint (Source: AAOS)
The two most comment indications for hip arthroscopy include the presence of symptomatic Femoroacetabular Impingment (FAI) or an acetabular labral tear.
FAI is a condition that affects the hip joint where there is abnormal contact between the femoral head and the acetabulum (hip socket) which leads to damage to the articular cartilage, the labrum, and the joint overall. There are three types of FAI (Figure 2), cam impingement, pincer impingement, and mixed impingement (cam and pincer combined). Cam involves an excess of bone along the upper surface of the femoral head. In this case, the bone is not round and thus cannot rotate smoothly inside the socket/acetabulum. This causes grinding to the cartilage inside the acetabulum. Pincer impingement is due to extra bone extending out over the normal rim of the acetabulum which can cause damage to the labrum. Mixed impingement just means that both the pincer and cam types are present. FAI causes increased friction between the acetabulum and the femoral head, resulting in pain and reduction of hip function.
Figure 2: Left is pincer impingement and right is cam impingement. (Source: AAOS)
Hip arthroscopy can be used to reshape the femoral head or acetabulum to prevent impingement and protect the hip from developing osteoarthritis (wear and tear, break down of cartilage).
The labrum can be damaged or torn. Damage to the labrum is usually associated with FAI but can also be caused by trauma or a high load/stress when trying to maintain coverage of the joint. During hip arthroscopy, the labrum can be debrided (removing damaged tissued), grafted, or repaired.
During the surgery, the patient is provided with a special boot to apply traction to the leg. This separates the bones of the hip joint, providing room for the surgeon to make a small puncture in the hip and insert the arthroscope. Initially, air and/or fluid is injected into the hip under the guidance of an x-ray. After the arthroscope is placed, two to four small 5-10 mm incisions are made at the side of the hip. Instruments are inserted through these incisions and through the arthroscope the surgeon can judge the condition of the hip, identify the damage, and perform the appropriate procedure. Oftentimes, saline is pumped through the joint during the procedure to improve visualization and flush out debrided tissue. The surgeon may shave tissue, cauterize structures, and remove damaged pieces. Sometimes the surgeon may drill holes where the cartilage has been lost, inciting localized bleeding encourage the formation of new/repair cartilage. This technique is known as microfracture or picking. After the surgeon is done with the procedure, the hip is usually injected with local anesthetic (decrease pain because it is an ambulatory surgery, the patient may leave the hospital as an outpatient) and the incisions are stitched or left to heal naturally.
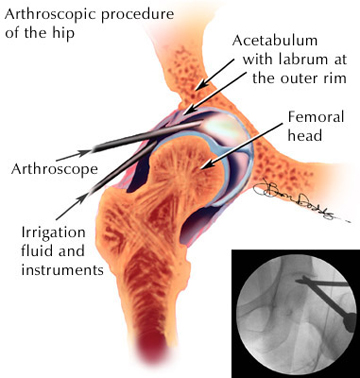
Figure 3: An image describing the arthroscopic procedure (Source: HSS)
THE INFECTION
After a loss to the Minnesota Wild on October 22nd, Rinne noticed soreness in his repair left hip. His soreness progressed to stiffness and a fever, leading to a diagnostic MRI and joint aspiration. A joint aspiration is when a need is inserted carefully into the joint to withdraw fluid which is then throughly tested for bacterial infections and other things. The aspiration and MRI confirmed that Rinne had an infection, so Rinne underwent another hip arthroscopy. However, the main objective of the surgery this time was to flush the joint (probably with saline and some antibiotics) and assess if there was any damage.
Infections following hip arthroscopies are extremely uncommon. While recognized as a risk with any surgery, there is less than a 1% change of infection following hip arthroscopies. Most follow-up studies following hip arthroscopy patients show no record of infection (Example of a Follow-Up Study), and even large scale surgeries such as knee arthroplasty (replacement) have small risk associated (Study Example).
Regarding hip arthroscopy, McCarthy et al. reported not a single case of septic arthritis in 1500 patients. This study goes as far as calling arthroscopy a "no problem surgery," stating that out of 2,640 patients that received the surgery, only 216 had complications post surgery (8.6%). Of those 216, only 126 were major complications, with just a few being infections. Another study had 4,256 arthroscopies with only 18 patients (0.42%) had an infection. The investigators believe that occurrence of infection is strongly associated with user of long-acting corticosteroids, longer operating times, increased procedures during the arthroscopy, prior procedures and the surgeon performing soft tissue debridement. Additionally, none of the infections were caused by E. coli, most originated due to Staphyloccocus aureus (MRSA). Patients in this study also had onset of symptoms (fever, etc) within 3 days of surgery, not five months.However, long-term results were successful, 17 of the 18 patients had a successful regimen of intravenous antibiotics.
Septic arthritis is seen as a major problem and one that could possibly lead to irreparable joint damage. It is especially dangerous in delayed diagnosed patients, where septic arthritis causes severe impairment of the affected joint and leads to a life threatening situation (Source).
It was revealed that Rinne's infection was a Escherichia coli infection. E. coli is one of the most frequent causes of many common bacterial infections. There are several different strains of E. coli and they have become increasingly difficult to deal with, due to an increasing resistance to common antibiotics. While E. coli is a common cause of infection in surgical wounds, especially abdominal operations, they are found sometimes found in other surgeries. It's doubtful that Rinne's E. coli infection is a bloodstream infection, it's almost certain that it is a healthcare or hospital-acquired-infection.
In an interview with Finnish magazine Urheilulehti, Rinne described the process and how the infection is an extreme setback and was actually life-threatening. Additionally, Rinne and his doctors are worried because the infection can cause permanent damage to the joint. The translated quotes from Rinne can be found here.
TREATMENT AND THE ROAD TO RECOVERY
First off, it's extremely odd that Rinne began having symptoms five months post surgery and was a surprise to many. For basic treatment, it is required that spend four to six weeks receiving antibiotics with a peripherally inserted central catheter (PICC) line in his arm for IV antibiotics. Studies show that the cornerstones of treatment is usually a multitude of strategies, including but not limited to mechanical purification, release of pressure in the joint, antibiotic therapy and functional healing. Fortunately, this regimen of antibiotics along with the flushing during his most recent hip arthroscopy works quite well according to many studies, such as this one .
I wish him the best and a good recovery. It's estimated that Rinne will miss 6-8 weeks now, putting him on track for a return around Christmas. Rinne's return would be a welcome present for Predators fans for sure.


The causes for hip pain when walking may be different for you and me. You may have arthritis in the hip which is just normal wear and tear of the joint tendon that eventually exposes the bone. You may have hip bursitis, or inflammation of the hip bursa. You may suffer from tendonitis, inflammation of the tendon in the hip joint.
ReplyDeleteaffordable knee replacement